Ocala Infectious Disease and Wound Center has been healing patients for over 11 years in Marion County. Their facility has grown over the last decade to meet the growing needs of the surrounding communities. What once started as a single physician practice treating infection related issues has now morphed into a comprehensive wound care clinic providing a multitude of services under one roof.
Within Ocala Infectious Disease’s wound care center, many diabetic patients have used their services for wound healing, infection treatment and limb salvage. According to the American Diabetes Association, diabetes affects 29 million Americans, and the number continues to rise each year due to America’s fast-paced lifestyle, leaving little room for healthy cooking, meals purchased ready-made or on the go, more sedentary lifestyles and sometimes poor choices ourselves.
People living with diabetes have an increased risk for loss of toes, feet or the legs. Elevated blood sugars within the body cause inflammation and damage to linings of arteries, which provides blood flow to the extremities and small capillaries in the skin, called microvascular disease. These persistent elevated blood sugars over time also cause neuropathy or loss of sensation to the extremities, particularly the feet. Neuropathy also affects the muscle structure causing collapse of arch in the feet leading to pressure and skin breakdown in areas that are not used to handling the weight of our bodies and changes in the glands of our skin, which become dry and do not produce proper oils for skin to remain soft and stretchy. This causes cracking and open wounds as well.
Once a wound occurs, the body’s protective mechanism, the skin, is lost and bacteria is able to get within the body, causing infection. Lower extremity infections are the most common reason for a diabetic to be admitted to the hospital, and these occurrences of ulcers and infection increase the risk of lower extremity amputation as well.
One may ask, “It’s just a toe. What’s the big deal if it gets removed? I have nine more.” But the answer is not that simple. If you are a diabetic and have your big toe amputated due to infection or a wound that won’t heal, you still have to heal the incision site left behind after the toe was removed. You still have the same risk factors that complicate wound healing, including loss of sensation and poor blood flow. The body has a miraculous way of adapting, and the second toe will grasp down on the ground for balance. The second toe, however, was not made to support that much weight, and if not careful, you can then develop an ulcer on the second toe, which then might also be amputated, and the third, and so on. Mayo Clinic notes that there is a higher risk of amputation after having an initial amputation. At Ocala Infectious Disease and Wound Center, this cascade of complications is what we work to prevent.
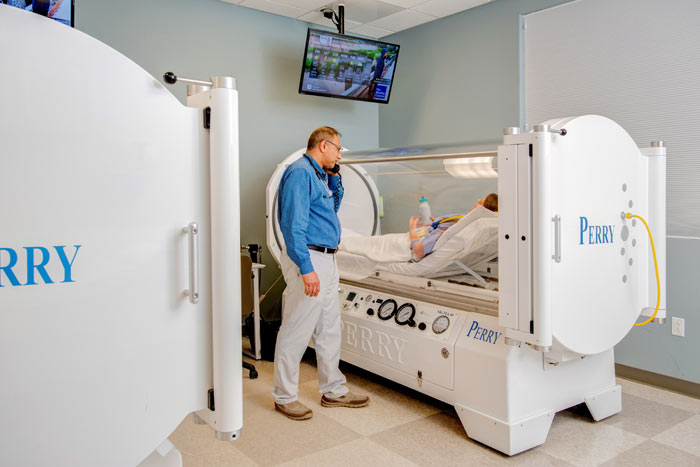
One of the latest ways of treating non-healing diabetic foot ulcers is hyperbaric oxygen therapy and Ocala Infectious Disease and Wound Center added the most up-to-date hyperbaric oxygen chambers to their new facility.
“Newer hyperbaric oxygen chambers are larger in size, allowing for better patient comfort. They are easily seen through, and the feeling of claustrophobia is really nonexistent. In our Perry Chambers, patients can even sit up, which helps with comfort, particularly when patients have difficulty lying on their backs. The success rate with hyperbaric oxygen therapy in combination of other care modalities is very high in our office,” says Lauren Mirza, ARNP.
The process of breathing 100 percent oxygen compared to only 21 percent, which is the percentage of oxygen we normally breathe, combined with pressure like you would experience whilescuba diving, allows oxygen to penetrate all body tissues, which is particularly important in diabetic wounds, as usually the small vessel blood flow to the skin is very poor. That is called microvascular disease. After about 21 days of treatment new blood vessels are created in the affected areas.
Hyperbaric oxygen therapy is somewhat of a commitment. The treatments happens five days a week for about two hours in and out the door. However, we try and remind patients that these smaller sacrifices, which only last a few months, may salvage a limb for a lifetime if followed up with good preventative care.
“We work to make coming into the office daily tolerable,” says Toby Cruikshank, HBOT technician. “We really treat patients like friends as well. I am beside the hyperbaric chambers at all times whenever a patient is in the chamber, and we can communicate freely back and forth through speakers. Most patients watch TV while getting their treatment, while others enjoy a good nap. Many times, if patients are unsure about doing hyperbaric, we even allow them to come and sit in the chamber and see how it feels without treatments so they will feel more comfortable. Whatever it takes for our patients,”
“We grew our practice under patient care,” Dr. Haris Mirza says.
“We don’t run through very quick, impersonalized visits. Our care is really comprehensive,” says Lauren Mirza, ARNP. “We care for them, as well as their problems. Initially, we were just treating infections, but much of the treatment came from getting that quality wound care. If you treat one aspect of a wound or infection but don’t address the other, it’s likely things will never get better. The fact that we can provide IV antibiotics, wound care, compression therapy for swelling, lab draws to monitor disease processes, vascular screening and hyperbaric oxygen therapy under one roof is big for us. We really do care.”
Statistics On The Diabetic Foot:
25% of patients will develop a foot ulcer at some time during their life.
2-6% of diabetics develop a wound yearly.
84% of non-traumatic limb amputations in diabetics are preceded by an ulcer.
34% of patients develop a new ulcer within one year of healing their first ulcer (70% at 5 years).
There is a 50% risk of developing a foot ulcer on the opposite foot after a major limb amputation, and a 50% risk of amputation of the remaining leg within 2-5 years.
The survival rate after a major limb amputation is 50% after three years and 40% after five years.
Measures For Preventing Diabetic Foot Ulcers:
Inspect your feet daily. If you cannot see the bottoms, use a mirror. Check in between the toes.
Wash your feet daily in lukewarm water, pat dry and remember to dry in between the toes.
Don’t remove callouses or other foot lesions yourself.
Trim your toenails carefully or ask your provider for assistance.
Never go barefoot.
Wear clean, dry socks.
Buy shoes that fit correctly. Avoid tight-fitting shoes, high heels and poor arch support. Most insurances will cover one pair of true diabetic shoes each year with a physician’s order.
Don’t smoke. Smoking worsens circulation and decreases oxygen in the blood.
Schedule regular foot checkups with Ocala Infectious Disease and Wound Center.
Take foot injuries or wounds seriously! Contact us if you have a foot sore that doesn’t heal quickly or becomes red, discolored or swollen. It is easiest to treat a wound early and prevent further complications.
We provide services at Munroe Regional Medical Center, Ocala Regional Medical Center, West Marion Hospital and Kindred Hospital and will be opening our NEW VILLAGES LOCATION by December 2016. If you or your loved one is in the hospital, please request the nurse or treating doctor for in-hospital consultation.
In addition to diabetic foot ulcers, we treat all open wounds on the body, boils or abscesses, skin lesions, surgical wounds, radiation related wounds, venous ulcers with edema, chronic lymphedema and more.
We also treat all infectious diseases, including reoccurring infections like UTI, recurrent lung infections, pneumonia, cellulitis, HIV, Lyme disease and more. Feel free to call our office for further questions.
Patients can be referred by a doctor or self-refer by calling our office.
Most insurances are accepted, including all Medicare and Medicaid plans, Freedom and BCBS. Call with any questions.
We will gladly work in collaboration to your current podiatrists, PCP and vascular doctors.






