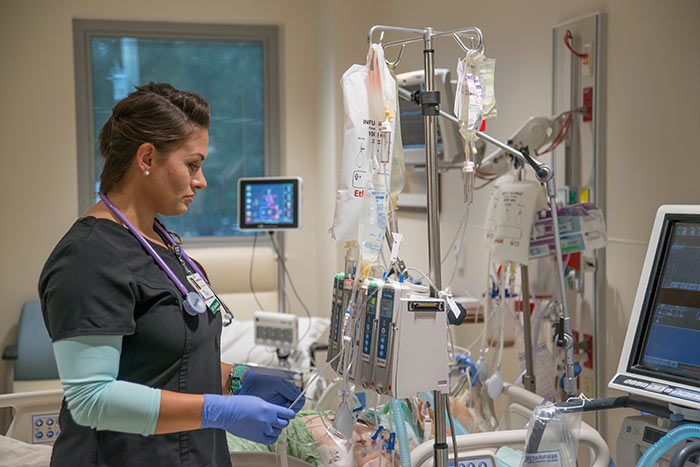
Nurses are critical contributors to getting patients healthy, the glue that binds each department together to treat someone in need. So what would it be like, as a newly graduated RN, to start your first day of work? Imagine trying to remember everything you’ve learned in nursing school while getting the hang of the hospital’s protocol and working with new machines. The transition is jarring at best. Now, Ocala Regional Medical Center has instituted a program that makes the transition a lot smoother.
Chief Nursing Officer Ann Szapor and Assistant Chief Nursing Officer Karen Henson began developing the Residency Program after Ann attended a conference in March 2015 for the American Organization of Nurse Executives, where she saw multiple presentations about residency programs for newly graduated nurses.
“This is becoming a recognized best practice nationally,” says Ann. “There’s so much for new nurses to learn in school, and when they come out of school, it’s difficult for them to put it all together. This allows them more structure and guidance from our education team and the nurses they’ll be working with.”
For all their time spent studying, new graduates have limited exposure to technological and regulatory issues, quality indicators or hospital-specific practices. Overwhelming seems like an understatement.
“This allows them to learn it before being put on the floor and taking a patient assignment,” says Ann.
The program’s inaugural class began their curriculum in July, with 12 residents specializing in medical-surgical nursing and six for the ICU. Nurse residents are hired as employees before they start the program. The program includes didactic components, online courses, simulations, observation and clinical time with a preceptor, an established nurse mentor.
Nurse resident Jennifer Roundtree certainly appreciated classroom debriefings after her shifts on the critical care unit.
“We’d have our two days of preceptorship [and] then come back, share our experiences and beef up on any skills we felt we should look up and discuss,” she says. Wanting to work in critical care, Jennifer knew this was the right program for her after graduating from Rasmussen in June.
“I was worried because most orientation processes are eight or nine weeks and then you’re on your own,” she says. “School doesn’t go over a fraction of the machines we use in critical care, so it’s a very daunting field to jump into when you’re just out of school.”
Each week, the nurses have two days with six to eight hours of class and two days of twelve-hour shifts on patient assignments with their preceptor. Those shifts are a time to explore the units of interest to them and learn from their mentors. They also complete online modules to refresh their education from nursing school and learn additional hospital-specific information.
“The nurse shadows the experienced nurse along the way, and over time, they give the patient assignment to the new nurse and begin to oversee them,” Ann explains.
Laura McKinney, director of education for Ocala Health, has done extensive research on the effectiveness of nurse residency programs for her final project in earning her Masters of Science in Nursing Education and was a main developer of the Residency Program.
“The first day they may just watch and follow, get used to the dynamic in the unit. Then, we may give them one patient or one task to be responsible for, like ‘today I’ll do all the care and you do all the documenting,’” says Laura. “We may give them two patients the first week or so, then move them up to three, then four, then, by the end, they have the whole assignment and we’re supervising.”
They also work on daily tasks that may be intimidating.
“We have grand rounds, and it’s the entire trauma team: pharmacy, dietary, the nurse practitioner, the PA, the surgeon. They all come in with their laptops and they’re ready for a report on their patient,” Jennifer says. “It can be a little intimidating to have them all around as you present this patient’s case. That’s when it’s great to have a preceptor there because she could fill in and back me up, and that has enhanced my communication and my thinking.”
Beyond standard duties, preceptors are always watching out for situations their residents have never seen before. Nurse residents all wear badges, so often other preceptors and staff will pull them into interesting experiences they see as learning opportunities.
“You’ve got a trauma coming in? Take my nurse resident; she needs to see how to receive a patient,” Laura explains.
Jennifer has had two preceptors due to schedule changes, but she enjoys the opportunity to learn from multiple mentors. Her first, Fran, was great at knowing when to let Jennifer take the lead on patient care and when to take over when Jennifer wasn’t ready. Yanique is teaching Jennifer about camaraderie and the teamwork aspect of nursing.
Besides helping the residents formulate their own nursing style, preceptors are key in connecting the new hires with the other employees. Laura remembers her first nursing position, which she began when the phrase ‘nurses eat their young’ was popular.
“One of the responsibilities of being a preceptor is to socialize your preceptee into the environment. When I was doing my research, I found a lot of articles addressing that as one of the most important things,” says Laura. “We have a family here, which is what I love most about Ocala Health.”
Jennifer says that support system is part of what helps her perform better compared to RNs not involved in a residency program.
“Several of my classmates are out on their own right now, and sometimes they seem like they’re overwhelmed because they don’t have the same backup. You can tell it affects how they feel about themselves and how they practice nursing.”
Overall the population in Ocala and surrounding regions is aging, so retaining higher numbers of well-trained nurses is vital. Just as important is empowering them and involving them in the hospital’s workings.
“For the hospital, it gives us the ability to stay ahead of our growth and be able to attract the best and the brightest,” Karen explains. Programs like this are few and far between, meaning many newly graduated RNs move away from the Ocala area to find them. ORMC is hoping to change that.
Dr. Barbara Lange, dean of nursing at College of Central Florida, says the program continues the feeling of having a safety net, allowing residents to ask questions without fear.
“They can still ask questions and have a procedure explained in a classroom instead of in front of a patient, where they may feel incompetent. I think it’s phenomenal because it helps students transition into the role of the nurse. They’re most likely to leave if the workload is too heavy or they’re not prepared,” she explains.
Karen Guty, DNP, RN and dean of nursing at Rasmussen, agrees, adding that confident nurses make for superior patient care.
“Ocala Health teams work hard to provide a service-focused, safe experience for patients. This is a structured way to bring that graduate nurse into a very complicated health environment and get them on solid footing so they’re able to do that and make significant contributions to patient care.”
The program is fluid, and the leaders are using residents’ feedback to improve it along the way.
“We would love to get them out to see what other departments do. They work with respiratory therapists, but I would like to see them get to go with one for part of a shift. I’d like to see them get an idea of how everything works together to get a patient well. The nurse is the one who is overall in charge of the patient, so they need to know what they do,” Laura says.
One thing that won’t change is instilling Ocala Health’s core purpose in each new nurse.
“I do a lot of training in customer service for nurses, and it all focuses on creating a special relationship with patients in addition to the clinical care we’re providing. It’s really about the personal touch and making a difference for our patients, making it a special experience for them,” says Ann.
The 18 nurses in the first residency class graduated in November and are already providing excellent care for patients inside ORMC. The next round of the program is slated to accept 12 new hires. As for Jennifer, whose residency ended November 30, she can’t wait to keep going to work every day with the other RNs on her unit.

“I’m really looking forward to feeling confident in standing on my own two feet, taking everything I’ve learned and putting it together. I don’t feel like a resident. I feel like I’m one of them already, and they’ve made me feel welcome on the unit. It’s knowing I can go in to work and save a patient if I need to, to troubleshoot, to work with the team. This program definitely helped build my skill set and also my confidence and camaraderie with my unit.”






